Air Force nurses serve in diverse positions at military medical treatment facilities throughout the country and around the world. They could be stationed anywhere from a large, multi-service hospital like Walter Reed National Military Medical Center in Bethesda, Maryland, or at a small family clinic like Eielson Medical Clinic at Eielson Air Force Base, Alaska.
As a family health clinic nurse, Air Force 1st Lt. Katelyn Schoneweis, a clinical nurse at Eielson, part of the 354th Healthcare Operations Squadron, explained how most of her focus is on dependents and retirees, but she also functions as a pediatric nurse due to the clinic's small size.
"My main focus is on the family health side, family members of active-duty and a lot of kids," said Schoneweis. "But with our clinic being so small, we help each other out often. So, I do see a good number of active-duty patients as well."
She added that being at an installation like Eielson allows her to see a wider array of patients than she might see at a larger facility, and that it's a good place to learn.
"That's kind of the cool thing about this clinic – with it being so small, we see a little bit of everything, from newborn babies to retirees," said Schoneweis. "It's good place to be for a newer nurse like me."
Schoneweis' only other duty station was Nellis Air Force Base in Nevada, where she worked in the inpatient medical/surgical unit for two years.
"This is a whole different realm in every aspect – moving from Las Vegas to Fairbanks, Alaska, my job, the environment. Everything here is completely different," she said.
In general, nursing provides the opportunity to branch out into areas that you may not have considered upon embarking on a career in medicine, she noted.
"Being a nurse, you can do so much in so many different positions, especially in the military because you're constantly moving," said Schoneweis. "It's been a great experience for me so far."
She compares her current position and her last one is to a civilian nurse going from working at a large hospital to a small family practice.
"I would think we do things pretty much the same, except that we're dealing with the military and dependents," she said.
The difference, she noted, is that service members, both patients and providers, are constantly moving, but that MHS GENESIS, the Military Health System's new, electronic health record, has helped immensely with the tracking of patients' medical histories.
"It's kind of a constant battle and one of the challenges we face in military health care. You don't have a set primary care provider. You have a provider for maybe three or four years and then start over somewhere else," said Schoneweis. "That's why we're so thankful for MHS GENESIS. It helps us keep much better track of our patients' medical history, past bases they've been at and gives us the ability to see their up-to-date health records."
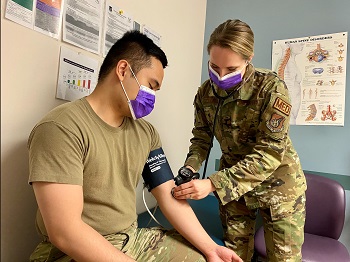 Air Force 1st Lt. Katelyn Schoneweis (right) checks the blood pressure of Air Force Senior Airman Neil Cariaga. Before working at Eielson Medical Clinic at Eielson Air Force Base, Alaska, Schoneweis, a clinical nurse, was at Nellis Air Force Base in Nevada for two years (Photo by: Courtesy Air Force 1st Lt. Katelyn Schoneweis).
Air Force 1st Lt. Katelyn Schoneweis (right) checks the blood pressure of Air Force Senior Airman Neil Cariaga. Before working at Eielson Medical Clinic at Eielson Air Force Base, Alaska, Schoneweis, a clinical nurse, was at Nellis Air Force Base in Nevada for two years (Photo by: Courtesy Air Force 1st Lt. Katelyn Schoneweis).
"It's been a huge help," she said. "It's fairly new to us. We just went through the transition in October, but so far, we're really liking the benefits."
Although it's still early in her career, Schoneweis said she's already been exposed to the benefits of working partnerships between departments and service branches, including sharing patients and specialty care with Department of Veterans Affairs hospitals when she was at Nellis, and now with Bassett Army Community Hospital at Fort Wainwright in Fairbanks, Alaska.
"They're a decent sized full-service hospital, so we end up interacting with them quite a bit," she said of Bassett "We use them as much as we can for hospitalizations as well as obstetrics care. We take care of our pregnant patients up until about 34 weeks and then we transition care over to Bassett because that's where they're going to end up giving birth."
She said the ability to care for their patients up to a certain point provides base residents the ease and convenience of being able to visit the clinic on base, where most of them live, and forego the 30-minute drive between Eielson and Wainwright until the final part of their pregnancy.
"It's good to have that connection and shared responsibility with the Army," she said.
Conversely, she said, a patient from Eielson who requires emergency room care would first go to Bassett and then be seen for any follow-up appointments back at Eielson.
"(MHS) GENESIS has helped immensely in this regard too because we can almost immediately see all of their emergency room records and we're not guessing what was done or constantly requesting records," said Schoneweis.
As with any service member, part of her work also entails maintaining readiness to be deployed. She said this has been accelerated by the arrival of F-35A Lightning IIs from the 356th Fighter Squadron to Eielson, which began arriving earlier this year. Schoneweis' husband is an F-35 pilot.
"The F-35s coming here turned Eielson into an operational base and our wing commander has been huge on readiness, not just for F-35 pilots, but the entire base," "We're always getting ready to go, when we need to go," said Schoneweis. "They've put the mindset on every squadron, including medical."
This includes a unique set of requirements for the clinic.
"For medical, that means making sure our airmen are always ready to deploy, staying up on immunizations, dental – making sure our personnel are good to go," she said.
A more operational mindset, she said, was facilitated not only by the arrival of the F-35 squadrons, but also by the COVID-19 pandemic.
"I think the pandemic kind of sparked that, probably for a lot of bases and people across the country, and we realized that maybe we weren't as prepared as we thought we were for something like this," said Schoneweis. "Now we know we need to be ready for anything that could happen."
In her eyes, constant training for real-life scenarios is the only way to prepare.
"Up here in interior Alaska, we're pretty isolated. We need to be able to take care of as many patients as we can to the greatest degree we can," she said. "COVID showed us that we can't wait for something to happen before we start training for it. If I'm getting deployed, I need to be flexible, ready and well-trained."